Understanding Hematomas: When a Bruise Is Something More Serious
Most of us have had a bruise — that familiar purple patch after bumping into a coffee table. But a hematoma is a fundamentally different, more serious event. At Vein Treatment Centers of NJ, we regularly evaluate patients who dismiss significant hematomas as "just a bad bruise," sometimes missing an important warning sign about their underlying vascular health.
This guide explains exactly what a hematoma is, how to recognize when yours requires medical attention, and why patients with venous disease are at significantly higher risk.
Bruise vs. Hematoma: What Is the Actual Difference?
Both involve blood escaping from damaged vessels, but the scale and consequences are very different.
A Standard Bruise (Ecchymosis)
- Involves tiny capillaries — the smallest blood vessels in the body
- Blood seeps into superficial layers just beneath the skin
- Appears as a flat discoloration that changes from purple to yellow as it heals
- Typically reabsorbs within 1–2 weeks without intervention
- Does not form a distinct lump or mass
A Hematoma
- Involves larger blood vessels — arteries, veins, or deeper capillary beds
- Blood actively pools and clots in a localized collection outside the vessel
- Forms a distinct, palpable lump that is often firm or fluctuant
- Can occur deep within muscle tissue, under the periosteum (bone covering), or in organ spaces
- May require drainage, medical management, or investigation of the underlying cause
The key distinction: a hematoma involves enough blood loss to form a contained collection, not just surface staining.
Recognizing the Symptoms of a Hematoma
A hematoma is not always immediately obvious. Learn to identify these warning signs:
Visual Signs
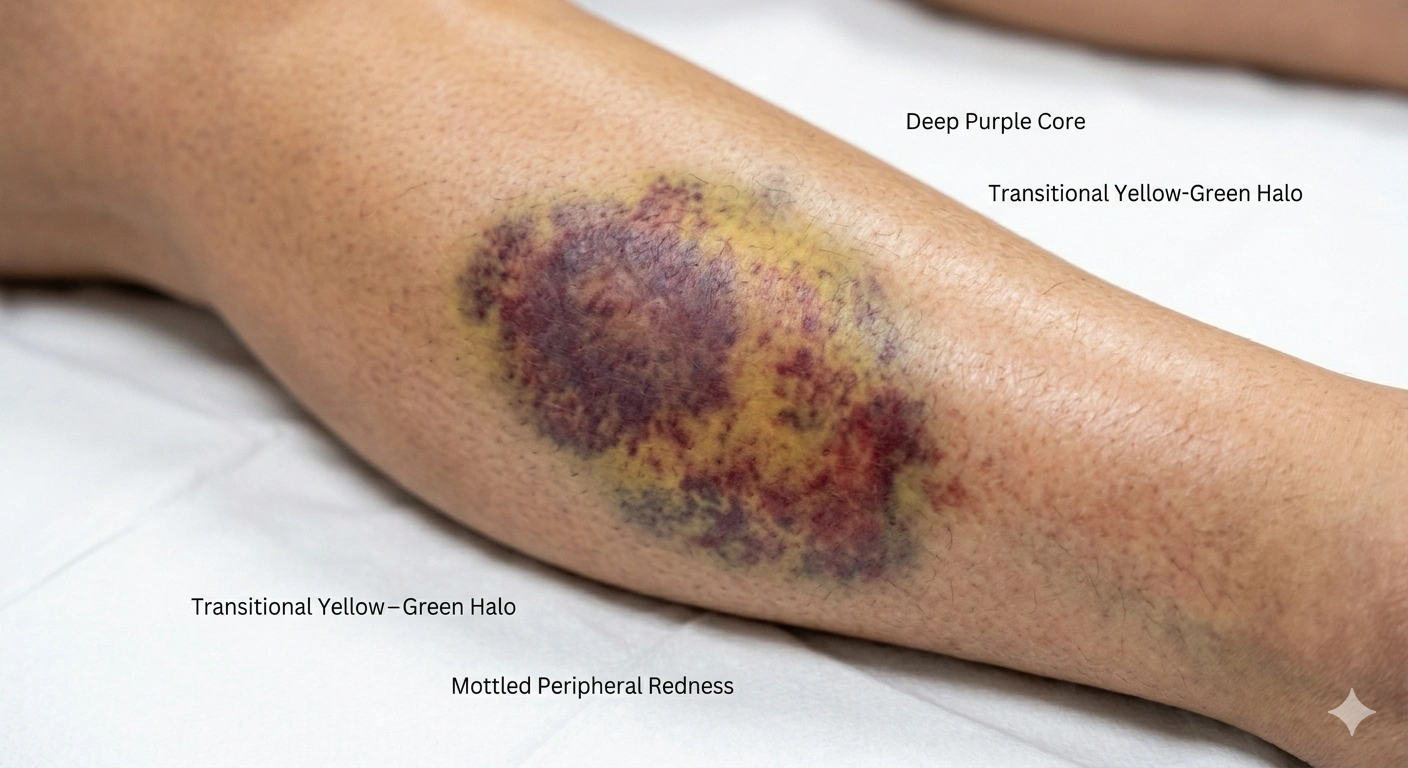
- Deep, dark discoloration — purple, maroon, or almost black patches that extend beyond the point of impact
- Spreading bruising — the discoloration enlarges over hours or days as blood tracks through tissue
- Skin tautness — the overlying skin may look shiny and stretched from the pressure of the blood collection
Physical Symptoms
- A firm or spongy lump under the skin — this is the clotted blood collection itself
- Significant throbbing pain — different from the dull ache of a bruise; a hematoma creates pressure on surrounding nerves
- Warmth — the area may feel noticeably warm due to inflammation
- Swelling and tension — the limb or body region may feel "full" and tight
Warning Signs That Demand Immediate Care
- Rapidly expanding hematoma — indicates ongoing arterial or venous bleeding that will not self-resolve
- Numbness or weakness in the limb — the blood collection may be compressing a nerve (compartment syndrome)
- Fever + increasing redness — signs of infection within the hematoma (rare but dangerous)
- Hematoma following a deep vein thrombosis diagnosis — if you are on blood thinners, hematomas can become serious very quickly
Why Patients with Vein Disease Are at Higher Risk
This is a critical connection that many patients — and even some primary care providers — overlook. Varicose veins and venous insufficiency significantly increase your susceptibility to hematomas.
How Diseased Veins Lead to Hematomas
- Weakened vein walls — chronic venous hypertension stretches and thins the walls of varicose veins, making them far more fragile than healthy vessels
- Superficial location — varicose veins sit just under the skin and are vulnerable to even minor trauma
- High internal pressure — the pooled blood in a varicose vein is under elevated pressure, so when the wall breaks, bleeding is more forceful
- Poor healing environment — chronic venous insufficiency impairs tissue oxygenation, slowing the body's ability to reabsorb a hematoma
At Vein Treatment Centers of NJ, we see patients who have suffered spontaneous rupture of a varicose vein — bleeding that begins without any trauma at all. This is a medical emergency. If you see blood suddenly appearing on your leg from a vein rupture, apply firm direct pressure and call 911.
Hematomas After Vein Procedures
It is also important to understand that small hematomas at injection or catheter insertion sites are a normal part of recovery after sclerotherapy, RFA, or ambulatory phlebectomy. These procedure-related hematomas:
- Typically appear within 24–72 hours of treatment
- Are usually tender but not severely painful
- Resolve on their own within 2–4 weeks
- Can be managed with gentle warm compresses after the first 48 hours
However, a hematoma that is growing, deeply painful, causing skin color changes, or triggering numbness should be evaluated promptly by our team.
Medical Treatment Options for Hematomas
Conservative Management (Most Cases)
- RICE protocol initially: Rest, Ice (first 48 hours), Compression, Elevation
- Warm compresses after 48 hours to promote reabsorption
- Compression wrapping to reduce swelling and prevent expansion
- Pain management with acetaminophen (avoid NSAIDs if on blood thinners)
Medical Intervention (Severe Cases)
- Needle aspiration — using ultrasound guidance to drain liquefied blood from the collection
- Surgical drainage — for large, organized hematomas that cannot be aspirated
- Treatment of the underlying cause — addressing the vascular disease responsible for the fragile vessels
Preventing Future Hematomas: Treat the Root Cause
If you have experienced multiple hematomas or a hematoma from very minor trauma, the underlying cause is almost certainly venous disease. Treating varicose veins and venous insufficiency with modern minimally invasive procedures does more than improve appearance — it strengthens the vascular system and dramatically reduces your risk of future complications including hematoma, bleeding, and ulceration.
Don't accept repeated bruising and hematomas as "just the way it is." Our team at Vein Treatment Centers of NJ can identify and treat the vein disease that is making you vulnerable. Call us today at 609-585-4666 for a comprehensive vascular evaluation. Learn more about how chronic venous insufficiency treatment can protect your vascular health long-term.
For informational purposes only. Not medical advice.