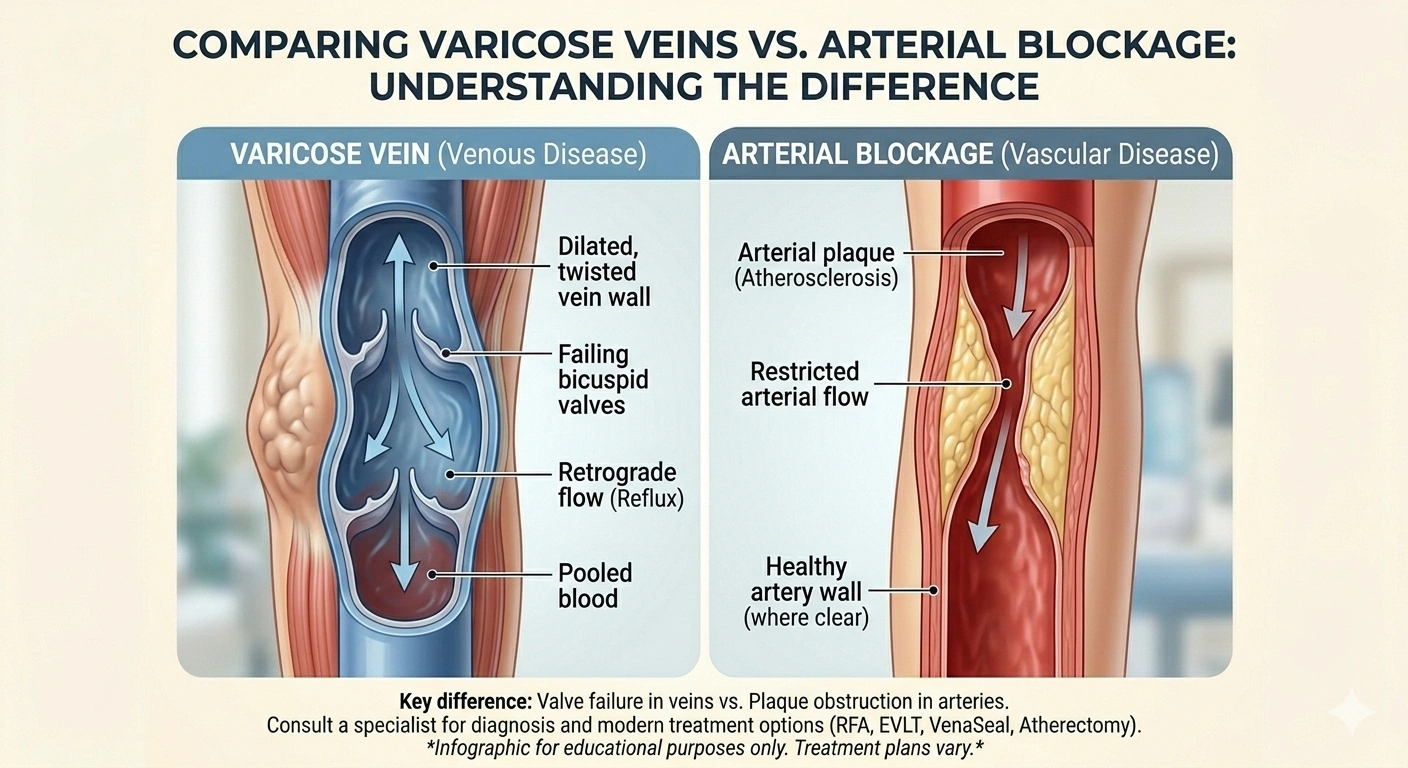
Peripheral Vascular Disease vs. Varicose Veins: Understanding the Critical Difference
Many patients arrive at Vein Treatment Centers of NJ having searched "vascular disease" and found themselves confused about whether they have a vein problem, an artery problem, or both. It is an understandable source of confusion — the terms "peripheral vascular disease," "vein disease," and "varicose veins" are often used interchangeably in casual conversation, but they describe entirely different medical conditions that require completely different treatments.
Getting this distinction right is not just academic — misidentifying your condition can lead to treatments that don't work or, in some cases, treatments that are actively harmful.
The Circulatory System: Two Separate Pipelines
Your legs contain two distinct types of blood vessels, each serving a separate function:
The Arterial System: Delivery
Arteries carry oxygen-rich blood from your heart down to your legs. They are high-pressure vessels with thick, muscular walls designed to withstand the force of each heartbeat. When arteries narrow due to atherosclerosis (plaque buildup), the condition is called:
- Peripheral Artery Disease (PAD) — the most common form of PVD
- Arteriosclerosis obliterans — in severe cases
The Venous System: Return
Veins carry oxygen-depleted blood from your legs back up to your heart. They are low-pressure vessels that depend on one-way valves and the pumping action of your calf muscles to move blood against gravity. When valves fail, the condition is called:
- Chronic Venous Insufficiency (CVI)
- Venous reflux disease
Varicose veins are the visible manifestation of venous insufficiency — enlarged, rope-like veins that form when blood pools due to incompetent valves.
Peripheral Artery Disease: Symptoms and Warning Signs
PAD is caused by atherosclerosis — the same plaque-forming process that causes heart attacks and strokes. The hallmark symptoms reflect inadequate oxygen delivery to the muscles:
- Claudication — cramping, aching, or fatigue in the calves, thighs, or buttocks that occurs with walking and relieves within minutes of rest
- Cold feet and toes — reduced blood flow lowers the temperature of the extremity
- Pale or bluish skin discoloration — especially when the leg is elevated
- Slow-healing or non-healing wounds — particularly on the feet or toes
- Hair loss on the lower legs — a subtle sign of poor circulation
- Weak or absent pulse in the foot or ankle
In severe cases, PAD progresses to Critical Limb Ischemia (CLI) — a condition in which even resting blood flow is insufficient, causing severe pain at night and tissue death (gangrene). CLI carries a significant risk of amputation.
Venous Insufficiency and Varicose Veins: Symptoms and Warning Signs
Chronic venous insufficiency produces a completely different symptom profile driven by blood pooling rather than blood deprivation:
- Leg heaviness and aching that worsens throughout the day and improves with elevation
- Swelling (edema) in the ankles and lower legs, particularly in the evening
- Visible, bulging, ropey veins on the surface of the legs (varicose veins)
- Skin discoloration — brownish, reddish staining around the ankles from hemosiderin deposits
- Stasis dermatitis — dry, itchy, inflamed skin caused by chronic venous pressure
- Venous ulcers — open wounds near the ankles in advanced, untreated disease
- Restless legs syndrome — a frequent but underrecognized manifestation of venous disease
Note a critical difference: venous symptoms worsen with standing and improve with elevation. Arterial symptoms worsen with elevation (because gravity is needed to deliver blood) and improve with letting the leg hang down.
Why the Distinction Matters for Treatment
This is where the distinction becomes medically critical:
Compression Therapy: Safe for Veins, Dangerous for Arteries
Compression stockings are a cornerstone of venous disease management — they reduce swelling, support vein walls, and improve venous return. But in a patient with significant PAD, compression stockings can reduce arterial inflow below the critical threshold, worsening ischemia and potentially threatening limb viability.
This is why our team always performs an Ankle-Brachial Index (ABI) test before recommending compression therapy. The ABI compares blood pressure at the ankle to blood pressure at the arm — a ratio below 0.9 indicates arterial disease, and below 0.6 may represent a contraindication to compression.
Can You Have Both Conditions?
Absolutely — and it is more common than you might expect. Both conditions share risk factors including age, obesity, smoking, and inactivity. When PAD and CVI co-exist, management requires careful balancing of treatments that address venous disease without compromising arterial flow.
The Diagnostic Process at Vein Treatment Centers of NJ
When you visit us for leg symptoms, we never assume which system is affected. Our comprehensive evaluation includes:
- Venous duplex ultrasound — mapping your deep and superficial veins for reflux, obstruction, and valve function
- Ankle-Brachial Index (ABI) — ruling out significant arterial disease before applying compression
- Clinical examination — assessing skin quality, temperature, pulses, hair distribution, and wound characteristics
- Medical history review — identifying cardiovascular risk factors, medications, and family history
If our evaluation suggests arterial involvement requiring advanced management, we coordinate care with vascular surgeons while continuing to manage your venous disease appropriately.
Treatment Pathways
For Venous Disease
When the diagnosis confirms venous insufficiency or varicose veins, our minimally invasive treatment options include:
- Radiofrequency Ablation (RFA) and Endovenous Laser Treatment (EVLT)
- Ultrasound-guided sclerotherapy for smaller veins and tributaries
- Ambulatory phlebectomy for bulging surface varicose veins
- VenaSeal medical adhesive closure
For Arterial Disease
Arterial disease management typically involves:
- Aggressive cardiovascular risk factor modification (blood pressure, cholesterol, diabetes, smoking cessation)
- Supervised exercise programs to develop collateral circulation
- Antiplatelet medications to reduce clot risk
- Angioplasty or bypass surgery in severe cases
Take the Right First Step
The most important thing you can do if you have leg symptoms is get an accurate diagnosis. Treating yourself for venous disease when you have arterial disease — or vice versa — will not help and can cause harm. Let the specialists at Vein Treatment Centers of NJ determine exactly what is happening in your legs and build the right treatment plan for your specific condition.
If you are experiencing unexplained leg swelling, pain, skin changes, or visible veins, call us today at 609-585-4666 for a comprehensive vascular evaluation. We serve patients throughout Hamilton, Trenton, Princeton, and all of Mercer County, NJ.
For informational purposes only. Not medical advice.