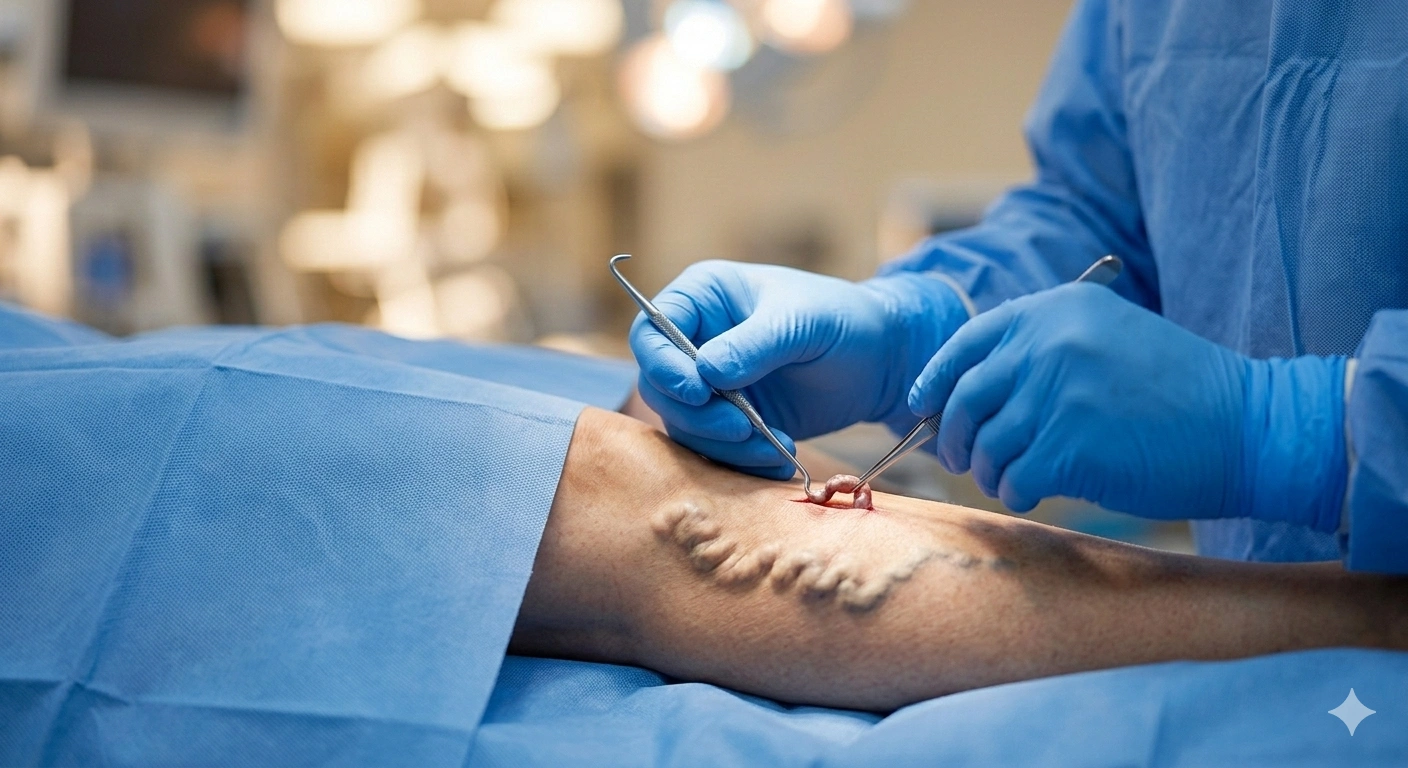
Ambulatory Phlebectomy: The Definitive Guide to Removing Large Varicose Veins
When varicose veins become large, rope-like, and visibly protruding, sclerotherapy alone is often insufficient and endovenous ablation (RFA or laser) treats the root cause but doesn't remove the bulge you can see and feel. This is the clinical scenario where Ambulatory Phlebectomy (AP) — also called microphlebectomy or stab phlebectomy — becomes the treatment of choice.
At Vein Treatment Centers of NJ, Dr. Hadaya performs ambulatory phlebectomy as an outpatient procedure that can be completed in under an hour, with patients returning to normal activity within 24–48 hours. This guide provides everything you need to know.
What Is Ambulatory Phlebectomy?
Ambulatory phlebectomy is a minimally invasive surgical technique that physically removes large, bulging varicose veins through a series of tiny, precisely placed skin punctures. The term "ambulatory" reflects the fact that patients walk in, walk out, and walk during recovery — no hospitalization, no general anesthesia, no bed rest.
The procedure was pioneered in Switzerland in the 1950s by Dr. Robert Muller, who refined it over decades into the technique used in leading vein centers today. It has an outstanding safety record and produces permanent removal of treated veins.
Why Large Varicose Veins Need Phlebectomy
Understanding why AP is sometimes necessary requires understanding what happens during endovenous ablation (RFA or EVLT):
- Ablation treats the root cause — it closes the incompetent great or small saphenous vein that is the source of venous reflux
- Once the pressure source is eliminated, smaller tributaries often shrink on their own over 3–6 months
- However, large, bulging tributaries — especially those with dilated diameters above 4–5mm — frequently do not shrink adequately after ablation alone
- These residual bulges can remain cosmetically unacceptable and may cause persistent symptoms
Ambulatory phlebectomy, performed either simultaneously with ablation or as a staged procedure 4–8 weeks later, removes these tributaries completely and permanently.
The Ambulatory Phlebectomy Procedure: A Detailed Walkthrough
Before the Procedure
During your pre-procedure appointment, Dr. Hadaya uses a skin marker to carefully trace and map the varicose veins that will be removed. This mapping is performed with the patient standing so gravity fills the veins to their maximum diameter, making the path of each vein clearly visible. Photographs are taken for documentation.
Anesthesia: Local Only
One of the most patient-friendly aspects of ambulatory phlebectomy is that it requires only local anesthesia. A series of small injections of lidocaine numb the skin and subcutaneous tissue along the mapped vein segments. There is no IV sedation, no general anesthesia, no anesthesiologist required.
For longer procedures treating extensive areas, a tumescent anesthesia solution (dilute lidocaine in saline) is infused around the veins for more comprehensive numbing and to minimize bruising.
Micro-Incision Placement
Once the area is completely numb, Dr. Hadaya makes a series of tiny punctures or "stab" incisions — each approximately 1–2mm in length — at intervals along the mapped vein path. These micro-incisions are so small that they:
- Do not require stitches or sutures
- Are closed with small adhesive strips (Steri-Strips)
- Heal to essentially invisible scars within a few months
- Leave no significant cosmetic scarring in the vast majority of patients
Vein Removal
Through each micro-incision, Dr. Hadaya uses a specialized phlebectomy hook instrument to grasp, elevate, and pull out a segment of the varicose vein. The technique involves:
- Inserting the hook through the incision and passing it alongside the vein
- Rotating the hook to snare the vein wall
- Gently withdrawing the vein segment through the incision
- Clamping and cutting the vein segment, then repeating at the next incision point
The procedure systematically removes the entire targeted varicose segment through these tiny access points. Most patients feel tugging or pressure during the vein extraction but no significant pain due to the local anesthesia.
Closure and Compression
After all targeted vein segments are removed:
- Micro-incisions are closed with adhesive strips
- A foam padding is placed over the treated area
- A medical-grade compression stocking or bandage is applied immediately
- The patient walks a short distance to confirm normal function and comfort
Recovery After Ambulatory Phlebectomy
First 24 Hours
- Keep the compression bandage or stocking in place continuously
- Walk gently for 15–20 minutes every 2–3 hours to promote healing
- Elevate the leg when sitting or resting
- Expect bruising and mild swelling — completely normal and expected
- Mild analgesics (acetaminophen) for any discomfort if needed
Days 2–7
- Transition to a compression stocking worn during daytime hours
- Return to work in most cases within 24–48 hours (desk work) or 3–5 days (physical labor)
- Continue daily walking
- Avoid strenuous exercise, heavy lifting, and hot baths for one week
- Keep micro-incisions dry for 48 hours; normal showering thereafter
Weeks 2–8
- Bruising fades progressively
- A firm cord may be palpable along the treated vein path — this is the healing tissue, not a problem
- Compression stocking wear as directed (typically 2–4 weeks total)
- Return to all normal exercise and activities at 2 weeks
- Follow-up ultrasound at 4–6 weeks to confirm complete vein removal and check for any residual veins
Ambulatory Phlebectomy vs. Traditional Vein Stripping: A Critical Comparison
If you have heard older patients describe "vein surgery," they are almost certainly describing vein stripping — the procedure that ambulatory phlebectomy has largely replaced. Understanding the difference helps explain why modern treatment is so dramatically superior:
- Vein Stripping: Required general anesthesia, hospital admission, groin incisions, and a wire threaded through the entire saphenous vein to strip it from the leg. Recovery took 2–6 weeks with significant pain and scarring.
- Ambulatory Phlebectomy: Local anesthesia only, outpatient office procedure, micro-incisions requiring no sutures, return to activity in 24–48 hours, minimal scarring.
Combining Phlebectomy with Ablation: The Complete Solution
For most patients with both a refluxing saphenous vein and large tributary varicosities, the optimal treatment combines both approaches:
- Endovenous ablation (RFA or EVLT) closes the incompetent saphenous vein — eliminating the pressure source
- Ambulatory phlebectomy removes the large, bulging tributary varicosities — delivering the visible cosmetic result
This "inside and out" combination is the gold standard approach for comprehensive varicose vein treatment, addressing both the anatomical cause and the cosmetic result in a single treatment visit or two closely spaced visits.
Is Ambulatory Phlebectomy Covered by Insurance?
When varicose veins cause documented symptoms (pain, swelling, skin changes, bleeding) and are associated with venous insufficiency confirmed on ultrasound, ambulatory phlebectomy is typically covered by Medicare and most major insurance plans as a medically necessary procedure. Our team handles all insurance verification and prior authorization on your behalf.
Schedule Your Consultation
If you have large, bulging varicose veins that are causing pain, affecting your appearance, or limiting your activities, ambulatory phlebectomy may be the right solution. Don't let bulging veins hold you back.
Contact Vein Treatment Centers of NJ at 609-585-4666 to schedule your consultation with Dr. Hadaya. We will evaluate your veins with diagnostic ultrasound, explain all treatment options, and design a personalized plan to give you the healthy, clear legs you deserve.
For informational purposes only. Not medical advice.